07/16/2010
During this final installment of our 3 part series about women and heart disease we will be focusing on heart problems older women are more likely to experience. Some of the things we will discuss are heart failure, diastolic dysfunction, atrial fibrillation, aortic valve disease and sudden cardiac death.

 7 Comments |
7 Comments |  "heart attack", atrial fibrillation, Blood Pressure, Depression, Go Red, healthy food, Heart Disease, Heart failure, Heart Health, Heart Healthy Diet, heart rate, Heart Truth, heartstrong, high blood pressure, hypertension, irregular heart beat, Ischemic stroke, Menopause, sudden cardiac death, sudden death, Women and Heart Disease, Women and Stroke, Women's Health | Tagged: "heart attack", afib, aortic stenosis, atrial fibrillation, cardioversion, catheter ablation, congestive heart failure, Heart Disease, Heart failure, sudden cardiac death, sudden death, Women and Heart Disease |
"heart attack", atrial fibrillation, Blood Pressure, Depression, Go Red, healthy food, Heart Disease, Heart failure, Heart Health, Heart Healthy Diet, heart rate, Heart Truth, heartstrong, high blood pressure, hypertension, irregular heart beat, Ischemic stroke, Menopause, sudden cardiac death, sudden death, Women and Heart Disease, Women and Stroke, Women's Health | Tagged: "heart attack", afib, aortic stenosis, atrial fibrillation, cardioversion, catheter ablation, congestive heart failure, Heart Disease, Heart failure, sudden cardiac death, sudden death, Women and Heart Disease |  Permalink
Permalink
 Posted by heartstrong
Posted by heartstrong
12/02/2009

An implantable cardiac defibrillator (ICD) is a small device that is implanted in the chest to help correct irregular life threatening heart rhythms (ventricular tachycardia or ventricular fibrillation). When the heart starts beating abnormally the ICD delivers an electrical impulse to the heart to shock it back into a normal heart rhythm. Patients with a weakened heart muscle (congestive heart failure) due to irregular pathways of caused by a heart attack, cardiomyopathy or high blood pressure are at risk for irregular heart rhythms. Research studies have shown that patients with irregular heart rhythms (ventricular tachycardia, ventricular fibrillation) are less likely to die suddenly after they receive an ICD. Many of these studies have included mostly men. So what is the impact of ICDs on a woman’s survival?
A study published in the Archives of Internal Medicine (2009) found that women with heart failure were just as likely to die with an ICD as women who did not receive the device. Men in the study had a 22% lower risk of dying if they had an ICD. But no benefit was observed in women with the ICD. The researchers suggest that because women are less likely to die from sudden irregular heart rhythms than men they are less likely to benefit from an ICD. Women are more likely to die from other causes. Since this study looked at the risk of death from any cause the results need to be reviewed with caution. Women who are candidates for an ICD should not be alarmed by the findings of this one study, clearly more data is needed. Women need to discuss their individual benefits and risks with their physicians to determine the most appropriate treatment.
For more heart healthy info visit http://www.heart-strong.com
 3 Comments |
3 Comments |  "heart attack", Heart Disease, Heart failure, Heart Health, heart rate, men and heart disease, sudden cardiac death, Women and Heart Disease | Tagged: arrhythmia, cardiac defibrillator, ICD, impantable cardiac defibrillator, irregular heart beat, irregular heart rate, irregular heart rhythm, sudden cardiac death, sudden death, Vfib, VTach, Women |
"heart attack", Heart Disease, Heart failure, Heart Health, heart rate, men and heart disease, sudden cardiac death, Women and Heart Disease | Tagged: arrhythmia, cardiac defibrillator, ICD, impantable cardiac defibrillator, irregular heart beat, irregular heart rate, irregular heart rhythm, sudden cardiac death, sudden death, Vfib, VTach, Women |  Permalink
Permalink
 Posted by heartstrong
Posted by heartstrong
09/27/2009
ECGs should be a routine part of every adult’s annual physical exam. ECGs can help identify heart muscle damage, heart enlargement and irregular heart rhythms. A new study published in the August 2009 edition of The European Heart Journal states that ECGs may also be able to help identify people at risk for Sudden Cardiac Death (SCD). The study suggests that increases in the QRS duration (the electrical activity from the ventricles, which are the bottom chambers of the heart) are significant predictors of SCD. The researchers in this study excluded patients with known causes of SCD (i.e.: bundle branch blocks or hypertrophy which is an enlargement of the heart muscle).
This is an interesting initial evaluation that needs to be investigated further but again stresses the importance of routine yearly exams. Men and women with a family history of SCD, stroke and heart disease especially may benefit from this routine screening. We just need to make sure our health care providers are aware of this relatively new predictor of SCD and send people on for further evaluation.
For more heart healthy info please visit www.heart-strong.com
 2 Comments |
2 Comments |  "heart attack", atrial fibrillation, heart rate, men and heart disease, Nursing, Premature heart disease, sudden cardiac death, Women and Heart Disease, Women and Stroke | Tagged: "heart attack", BBB, bundle branch block, ECG, electrocardiogram, fitness, Heart Disease, high blood pressure, SCD, sudden cardiac death, sudden death |
"heart attack", atrial fibrillation, heart rate, men and heart disease, Nursing, Premature heart disease, sudden cardiac death, Women and Heart Disease, Women and Stroke | Tagged: "heart attack", BBB, bundle branch block, ECG, electrocardiogram, fitness, Heart Disease, high blood pressure, SCD, sudden cardiac death, sudden death |  Permalink
Permalink
 Posted by heartstrong
Posted by heartstrong
07/07/2009
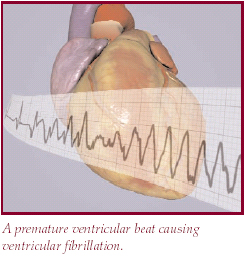
Sudden cardiac death (SCD) is the term used when someone dies suddenly from an irregular heart rhythm. Experts stated that approximately 10% of SCD is the result of an inherited heart condition. When a man or women under fifty years old died suddenly, autopsy results revealed that an inherited heart disorder was frequently present. Sudden cardiac death is one of the leading causes of death among young people, claiming approximately 3,000 lives per year.
The important message here is that first-degree relatives of SCD need to be screened for the presence of an inherited cardiac abnormality. Some inherited disorders can be managed with medications and lifestyle changes while others may require electrical devices (internal cardioverter defibrillator or ICD) or interventional procedures like a catheter ablation.
For more information visit:
http://www.nhlbi.nih.gov/health/dci/Diseases/scda/scda_whatis.html
http://www.hrspatients.org/patients/heart_disorders/cardiac_arrest/default.asp
www.heart-strong.com
 Leave a Comment » |
Leave a Comment » |  "heart attack", Children heart disease, genetic testing, Heart Disease, Heart disease young women, Heart Health, men and heart disease, Premature heart disease, Women and Heart Disease | Tagged: "heart attack", Heart Disease, SCD, sudden cardiac death, sudden death, Women and Heart Disease |
"heart attack", Children heart disease, genetic testing, Heart Disease, Heart disease young women, Heart Health, men and heart disease, Premature heart disease, Women and Heart Disease | Tagged: "heart attack", Heart Disease, SCD, sudden cardiac death, sudden death, Women and Heart Disease |  Permalink
Permalink
 Posted by heartstrong
Posted by heartstrong
04/14/2009
 With the recent push for increased physical activity, participation in triathlons has dramatically increased. Triathlons consist of a three-sport endurance event consisting of swimming, cycling and running. Many people who participate in these events come from a strong background in one of the sports and then train for the other two legs. A recent study demonstrated that the risk of sudden death in the triathlon was 1.5 per 100,000 participants. The study included 922,810 participants. There were a total of 14 deaths, 11 in men and 3 in women. Thirteen of the deaths occurred during the swimming leg of the race and were initially thought to be from drowning. Autopsies were performed on 6 of the 13 swimming deaths and underlying cardiovascular disease was found in 4 of them. Some possible reasons for the swim being the most dangerous leg included: cold water causing irregular heart rhythms, the inability for the athlete to stop and rest when he/she is in trouble and just inexperience in the water. The different triathlon distances did not have an effect on the death rates. In comparison, a study of 3 million marathon runners showed the sudden cardiac death rate to be 0.8 per 100,000 participants (almost ½ of the triathlon rate).
With the recent push for increased physical activity, participation in triathlons has dramatically increased. Triathlons consist of a three-sport endurance event consisting of swimming, cycling and running. Many people who participate in these events come from a strong background in one of the sports and then train for the other two legs. A recent study demonstrated that the risk of sudden death in the triathlon was 1.5 per 100,000 participants. The study included 922,810 participants. There were a total of 14 deaths, 11 in men and 3 in women. Thirteen of the deaths occurred during the swimming leg of the race and were initially thought to be from drowning. Autopsies were performed on 6 of the 13 swimming deaths and underlying cardiovascular disease was found in 4 of them. Some possible reasons for the swim being the most dangerous leg included: cold water causing irregular heart rhythms, the inability for the athlete to stop and rest when he/she is in trouble and just inexperience in the water. The different triathlon distances did not have an effect on the death rates. In comparison, a study of 3 million marathon runners showed the sudden cardiac death rate to be 0.8 per 100,000 participants (almost ½ of the triathlon rate).
 Leave a Comment » |
Leave a Comment » |  "heart attack", exercise, fitness, Heart Disease, Heart disease young women, Heart Health, men and heart disease, Premature heart disease, Women and Heart Disease | Tagged: "heart attack", "heart healthy", exercise, fitness, Heart Disease, Heart Health, heart healthy habits, marathon, role model, sudden death, triathlon |
"heart attack", exercise, fitness, Heart Disease, Heart disease young women, Heart Health, men and heart disease, Premature heart disease, Women and Heart Disease | Tagged: "heart attack", "heart healthy", exercise, fitness, Heart Disease, Heart Health, heart healthy habits, marathon, role model, sudden death, triathlon |  Permalink
Permalink
 Posted by heartstrong
Posted by heartstrong



 Posted by heartstrong
Posted by heartstrong 








